Using Social Determinants of Health to Combat COVID-19
With the total number of confirmed coronavirus cases around the world surpassing 4 million in May, COVID-19 has become one of the worst pandemics in history, and it all happened in what seems like the blink of an eye.
As coronavirus disease has ravaged the globe, there likely isn’t a single person who hasn’t experienced a change in their day-to-day life, especially in the United States. From stay-at-home and shelter-in-place orders across the US, to staggering unemployment numbers, to increased stress, anxiety and depression, we have all been thrown into a situation we never expected.
And yet, there is a segment of the population whose situation is worse than most—older adults and people with serious underlying medical conditions who are at higher risk for severe illness from COVID-19. Many of these individuals were already struggling with their health, and now, they must go to extreme lengths to protect themselves from the spread of coronavirus.
As healthcare organizations, we have the opportunity—and some would say, responsibility—to help those under increased threat from COVID-19. These individuals are confused and scared; they are isolated, they don’t know who to trust; and many don’t even know what to do if they get sick. What can we do to help?
The first step to providing support is figuring out who needs your help the most.
Can Predictive Analytics & Social Determinants of Health Help Fight COVID-19?
At present, there is limited information regarding the specific factors that increase risk for serious disease from COVID-19. Predictive analytics rely on historical patterns, both hidden and obvious. The industry does not have the history to identify such patterns with a novel disease like COVID-19.
Additional challenges in the application of this identification process arise due to the inconsistency among individuals and the seriousness of their coronavirus complications. Two individuals with nearly identical health histories and social determinants can experience vastly different levels of severity when exposed to COVID-19.
Still, Pareto has extensive client experience and claims history from the Pareto Community, as well as access to the clinical experts at Gorman Health Group, which allowed us to dig into the medical profiles of various populations. Based on what has been documented about COVID-19 to date, we identified a loosely targeted population who is more susceptible to serious complications from coronavirus disease. While the infection is clearly widespread, this level of insight can help a health plan or provider understand who—within their patient population or book of business—is at risk for hospitalization and take action to outreach to that person or resource/capacity plan accordingly.
Analyzing Risk of COVID-19 Complications
Leveraging the health history in our dataset, we have identified the medical conditions and social determinants of health (SDOH) contributing to a decline in overall health status that could potentially be worsened by a COVID-19 diagnosis. By combining this with external research and clinical input, we developed a process that identifies a population suspected as being at risk for serious COVID-19 complications.
This model considers the contributing factors for increased severity related to other respiratory viruses, as well as the progression of those infections, using outcomes from the Pareto Community. For example, through our analysis and model refinement, we found that a history of cancer and chemotherapy is the greatest risk factor contributing to the seriousness of complications from respiratory viruses. Additionally, Lupus and advanced kidney disease are significant contributors. We have incorporated these insights into our COVID-19 risk identification methodology, while also leveraging general health history, external research and clinical input.
Overall, the factors and characteristics that contribute to the identification of this population include, but are not limited to:
- Medical History:
- Diabetes
- Lupus
- History of cancer and chemotherapy
- End Stage Renal Disease (ESRD)
- Sickle-cell Anemia
- Anemia
- Depression and/or other mental health history
- Respiratory conditions
- Immunocompromised
- Alzheimer’s Disease
- Lifestyle/SDOH:
- History of homelessness
- Urban living
- Poor air quality
- History of smoking
- Recent and/or frequent traveler (international and domestic)
The outputs of the COVID-19 risk model identify members at a greatly elevated risk for severe complications and those at risk for hospitalization.
Below is a summary of the risk distribution for COVID-19 complications among the Pareto Community:
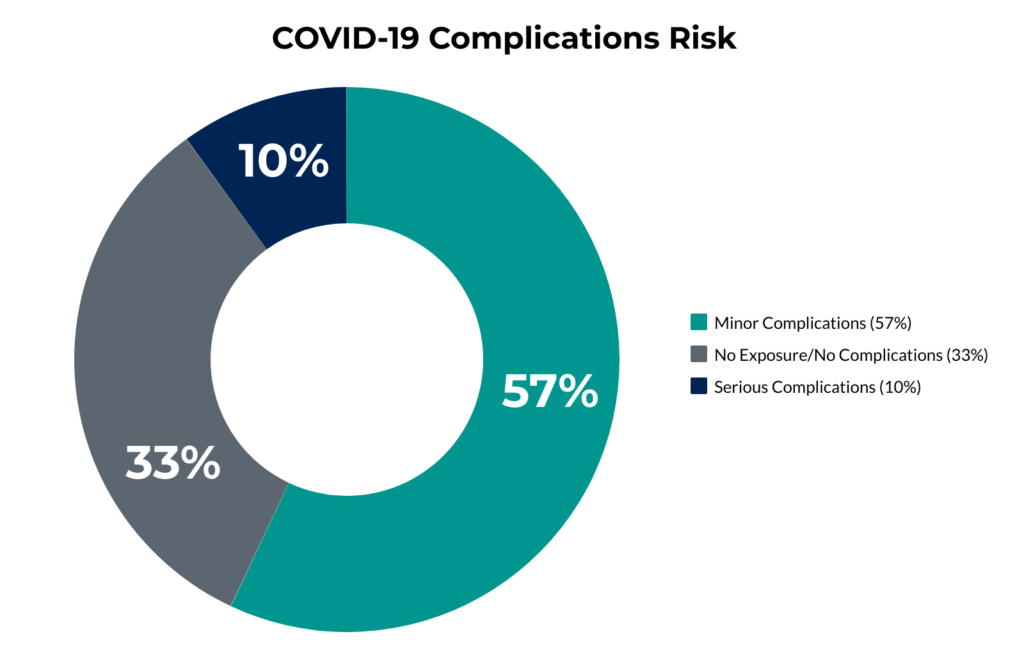
On average, around 10% of a health plan’s membership is prone to serious complications as a result of exposure to COVID-19.
While we are unable to assess the complete accuracy of our predictions, due to the limited supporting information available, this model relies on an extensive repository of medical claims, clinical input and analytics expertise that is sufficient to establish a baseline for outreach, follow up and general support for those struggling through this difficult time.
Conclusion
As healthcare organizations across the country do everything they can to keep their heads above water, relying on data and predictive analytics to create focus and allocate resources will establish certainty in an environment plagued by uncertainty. An analysis like this one from Pareto equips care and case management teams with additional insight into members, which will ultimately help these groups efficiently deliver the services people need to stay safe and healthy during this pandemic.
To complement this analysis, Pareto is collecting monthly data on the services and locations most impacted by COVID-19. A live version of this data is available here.
Our team of advisors consist of seasoned veterans who have served at every decision-making level of leading health plans. We’re dedicated to helping organizations grow, perform, and transform through professional consultancy and technology-based solutions. Contact us to learn more.
