Attack of the Clones: Using Clone Analysis & Predictive Algorithms to Profile Newly Enrolled Members
Pareto Intelligence applies advanced predictive analytics to deliver immediate and actionable insights into new member populations. For new ACA member populations in 2017, Pareto:
- Predicted PLRS within 1% of actual results, enabling more accurate transfer payment accruals.
- Stratified new members across condition and cost outcomes with over 90% accuracy, prioritizing health plan outreach to proactively engage targeted members in care management, risk and quality programs.
With continued year-over-year volatility in the Affordable Care Act (ACA) market, 2017 saw 129 plans exit the marketplace. These exits, paired with increasingly knowledgeable consumers willing to shop around on an annual basis, contribute to shifting relative risk for issuers. Even a small change in membership due to new enrollees can have a significant impact on risk scores. While plans use an abundance of data (medical claims, pharmacy claims, utilization patterns, etc.) to inform both risk adjustment outreach tactics and risk adjustment reserve levels, this data is only available for historical members. As such, plans are left with a blind spot regarding the impact from newly enrolled members.
With few data points to leverage, insurers have limited options to inform prioritization efforts for new enrollee outreach. Plans can end up spending far too many resources engaging new members with little diagnostic risk, or too few resources engaging and managing care for newly enrolled polychronic or diagnostically complex members. Likewise, new enrollee impact on risk scores remains an unknown, leaving plans to approximate needed reserve levels which, if underestimated, can have a costly and burdensome impact on the plan’s financial stability.
Existing tactics for understanding and engaging new members include issuing Health Risk Assessments (HRAs) upon enrollment and offering free or incentive-based initial wellness visits. However, return rates and turnaround times for completed HRAs vary and information contained on them still needs to be aggregated to produce insight for the plan. These assessments also rely on complete and accurate member disclosure of health status, risk behaviors, and utilization patterns, rather than on empirical diagnostic data. Considering these inefficiencies, Pareto sought to find a better way to predict the impact of newly enrolled members on a health plan’s book of business.
Profiling New-to-Plan Member Populations Through Clone Analysis
For the 2017 benefit year, Pareto Intelligence entered into an engagement with a new market entrant to mitigate the uncertainty regarding risk scores and financial impact from an unfamiliar book of business. While the client didn’t have historic information about its members, it was able to provide Pareto with a limited claims dataset spanning the first two months of 2017. Leveraging data from its extensive community, Pareto accurately predicted risk scores for its client’s individual risk pool within 1% of actual performance, which was confirmed by the ACA risk adjustment transfer payment results released on July 9.
By analyzing demographic information available from enrollment data and the limited 2017 claims data provided, Pareto matched plan enrollees to historical members within the Pareto Community, thus establishing a “clone” or a member demographically identical and statistically similar in terms of cost, utilization, and clinical profile.
Using this “clone” population and adjusting for Geographic Cost Factor, inflation between 2016 and 2017, and outliers, Pareto synthesized enrollment behavior, utilization behavior, and disease progression for its client’s members over the course of 2017, thereby predicting otherwise unknown cost and risk metrics. Using the output of this “clone analysis,” Pareto’s client estimated and set adequate reserve levels based on a unique empirical approach, ensuring they were appropriately prepared in the event of a transfer payment obligation.
Supplementing Clone Analysis with Benefit Selection
Applying a Clone Analysis to your newly enrolled population is a reliable method for synthesizing member behavior over the course of a year, but it relies on available diagnostic data. What about situations in which claims data is unavailable to power the analysis? Plans are often anxious to glean insights into their new members before claims data exists. To address this need, Pareto maintains a collection of algorithms not reliant on claims data to predict new member clinical and cost outcomes. This New Member Algorithm identifies behavioral patterns correlated to specific benefit selection. That is, it predicts, with ~90% accuracy, new members’ diagnostic acuity and associated costs solely based on their demographics and the benefit design of the products they purchase.
The New Member Algorithm differentiates between members predicted to have high costs but suspected to lack a risk adjustable chronic condition and possible poly-chronic members predicted to have high costs. With this information, plans can use the outputs of the algorithm to target those members suspected of having complex chronic or poly-chronic conditions for member outreach and encounter facilitation to ensure all existing chronic conditions are assessed and appropriately documented for risk adjustment. Likewise, plans can target potential high-cost new members for clinical care programs to better manage their care and the costs associated with it.
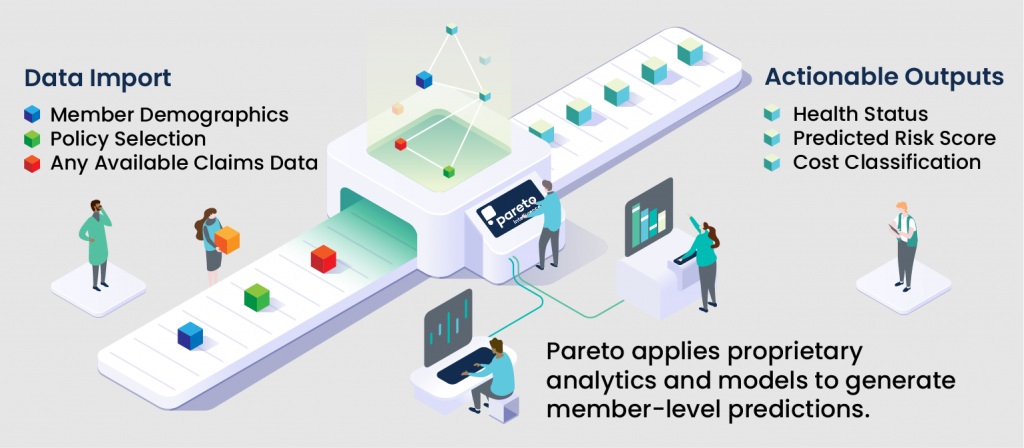
While both the Clone Analysis and the New Member Algorithm seek to address unknowns regarding a plan’s newly enrolled members, they do so leveraging different datasets. Used alone, each will provide insight into the costs and clinical status of new members. However, when supplementing the Clone Analysis with the New Member Algorithm, results are bolstered, and a more informative new member narrative is developed, allowing plans to feel more confident in decision-making and defining revenue management strategies.
Regardless of the extent of clinical and historical data available, there are irrefutable benefits to applying analytics to garner information about an unfamiliar population. At a minimum, having a macro-level understanding of one’s membership and its associated clinical complexity will better position plans to succeed in risk adjusted markets. With facilitated encounter season upon us, the Clone Analysis and New Member Algorithms are tools that can be deployed to prioritize members for outreach, allowing for increased risk documentation capture before the end of the benefit year.
